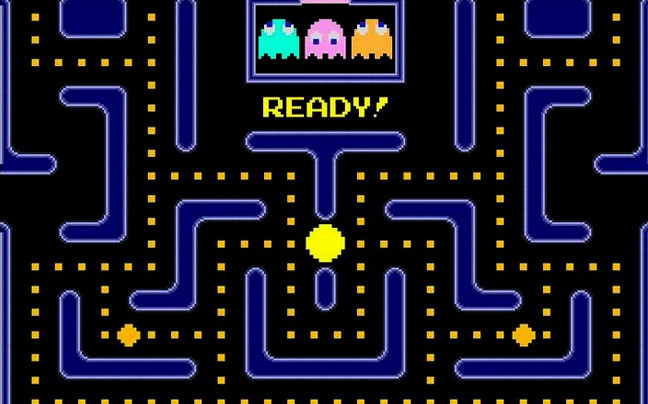
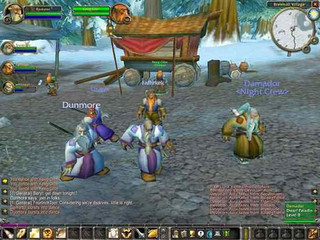
Η απίθανη ιστορία κατασκευής ενός από τα δημοφιλέστερα παιχνίδια όλων των εποχών! (ΦΩΤΟ) – Makeleio.gr
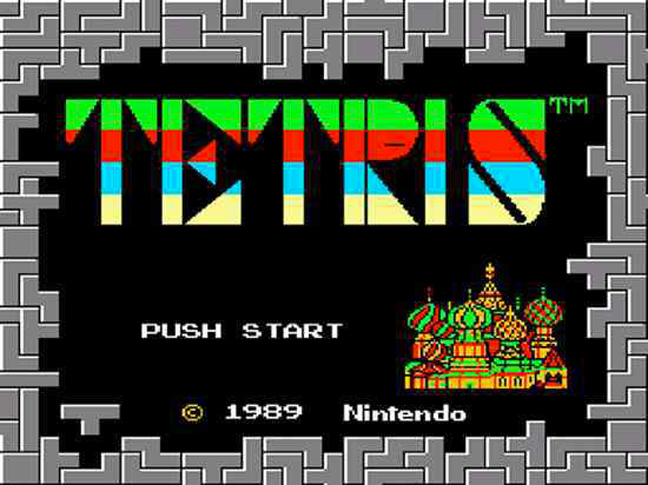
Ηλεκτρονικά παιχνίδια που έγραψαν ιστορία ~ ialmopia.gr | Τοπική ηλεκτρονική εφημερίδα ενημέρωσης και ψυχαγωγίας

Παιχνίδι χωρίς όρια, Ποδοσφαιρικές στιγμές που έγραψαν ιστορία - Χρήστος Σωτηρακόπουλος | Skroutz.gr
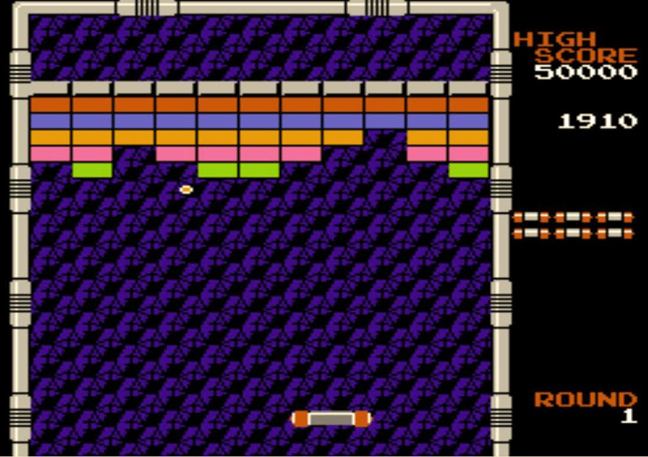
Ηλεκτρονικά παιχνίδια που έγραψαν ιστορία ~ ialmopia.gr | Τοπική ηλεκτρονική εφημερίδα ενημέρωσης και ψυχαγωγίας
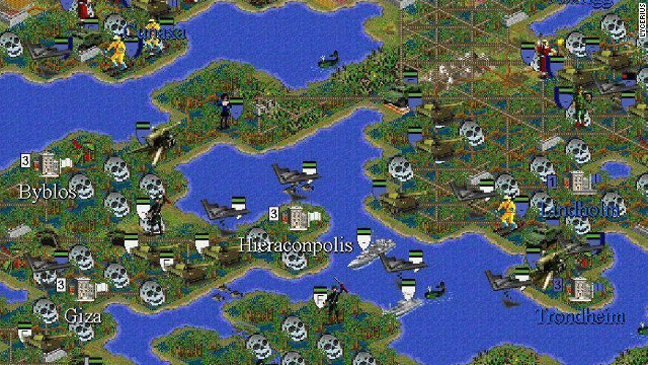
Ηλεκτρονικά παιχνίδια που έγραψαν ιστορία ~ ialmopia.gr | Τοπική ηλεκτρονική εφημερίδα ενημέρωσης και ψυχαγωγίας

Ηλεκτρονικά παιχνίδια που έγραψαν ιστορία ~ ialmopia.gr | Τοπική ηλεκτρονική εφημερίδα ενημέρωσης και ψυχαγωγίας
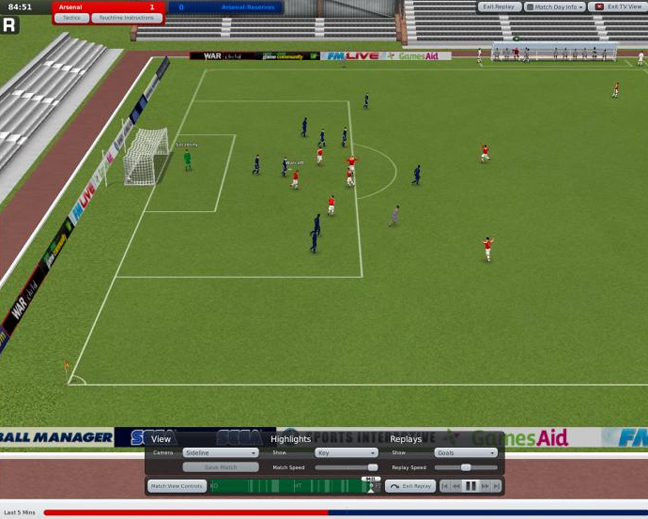
Ηλεκτρονικά παιχνίδια που έγραψαν ιστορία ~ ialmopia.gr | Τοπική ηλεκτρονική εφημερίδα ενημέρωσης και ψυχαγωγίας




/s3.gy.digital%2Fklapsinakis_gr%2Fuploads%2Fasset%2Fdata%2F99938%2F237.724_1.jpg)