
ΜΑΓΙΟ ΣΟΥΤΙΕΝ BIKINI TOP SANS COMPLEXE-S REFLET BRA WIRED CLASSIC 78AAH72-D-22 LUREX Μέγεθος (Σουτιέν) 85D Χρώμα Κεραμιδί

DD - Σουτιέν για Πολύ Mεγάλο Στήθος - Πολύ Μεγάλα Μεγέθη DD - DD+ E - F - G - H - I - Γυναικεία Εσώρουχα

Deep V - Σουτιέν για Πολύ Mεγάλο Στήθος - Πολύ Μεγάλα Μεγέθη DD - DD+ E - F - G - H - I - Γυναικεία Εσώρουχα

DD - Σουτιέν για Πολύ Mεγάλο Στήθος - Πολύ Μεγάλα Μεγέθη DD - DD+ E - F - G - H - I - Γυναικεία Εσώρουχα
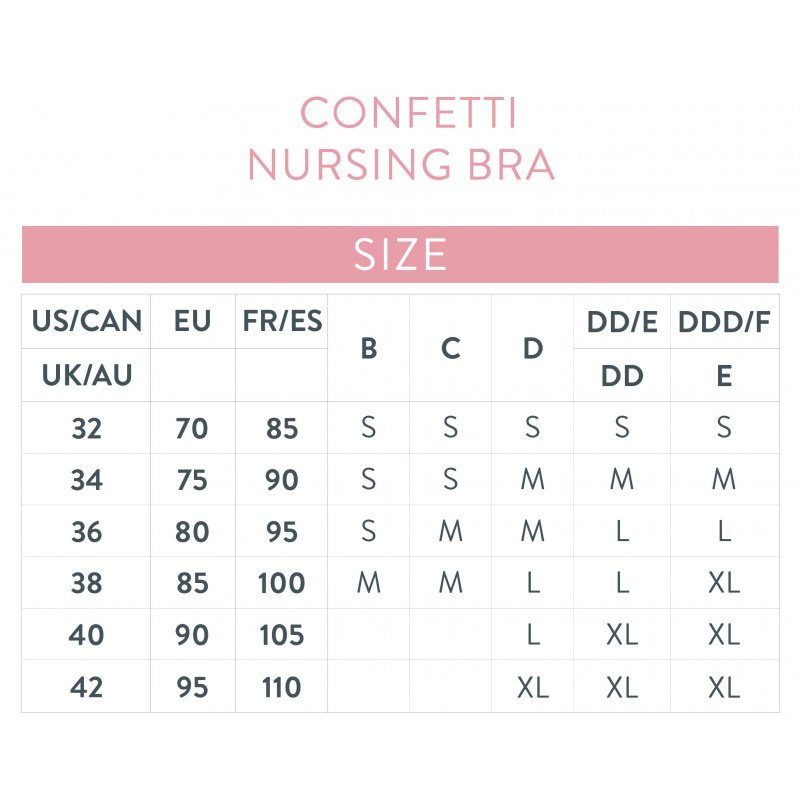
Bravado Confetti Σουτιέν Θηλασμού Μωβ με Λευκό Πουά Small | Βρεφικά Είδη – Βρεφικά Έπιπλα Σε Μοναδικές Προσφορές! | Anatello | chicco, stokke.

Beauwear Summer Ultra Thin Plus Size Minimizer σουτιέν για γυναίκες Χωρίς επένδυση Εσώρουχα CD DD E 38/85 40/90 42/95 44/100 46/105 48/110 - Badu.gr

DD - Σουτιέν για Πολύ Mεγάλο Στήθος - Πολύ Μεγάλα Μεγέθη DD - DD+ E - F - G - H - I - Γυναικεία Εσώρουχα















