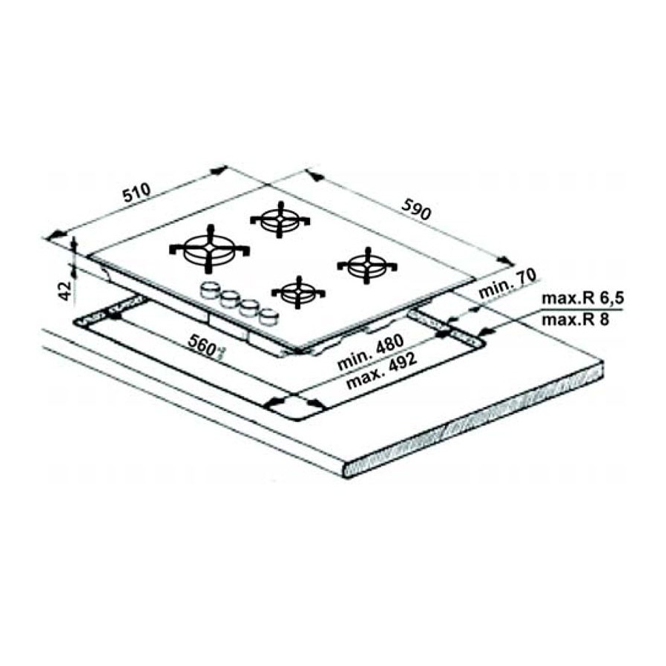
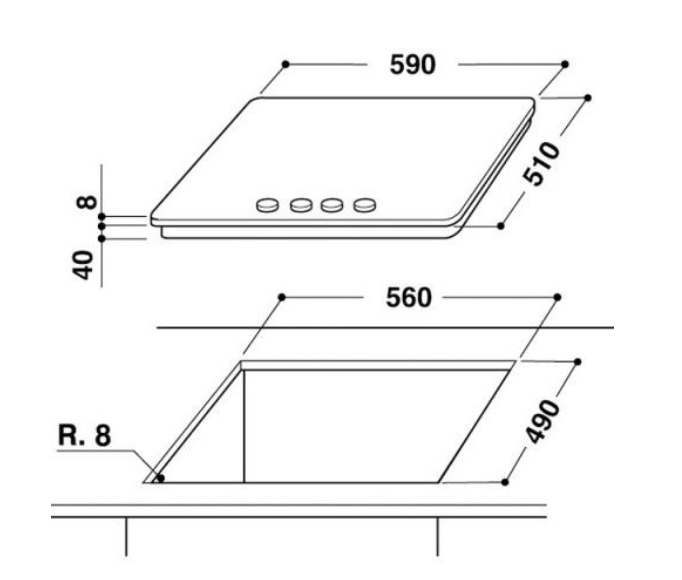
Варочная поверхность WHIRLPOOL GOR 6414/NB - Купить в Киеве, Украине • Лучшая цена в интернет-магазине - tehnohata.ua
Газовая варочная панель Whirlpool GOR 6414/NB - «Газовая варочная панель Whirlpool GOR 6414/NB отличная панель! Всем рекомендую» | отзывы

Whirlpool GOR 6414/NB купить в интернет-магазине: цены на варочная поверхность газовая GOR 6414/NB - отзывы и обзоры, фото и характеристики. Сравнить предложения в Украине: Киев, Харьков, Одесса, Днепр на Hotline.ua

Buy Whirlpool GOR 6414/NB / — in the best online store of Moldova. Nanoteh.md is always original goods and official warranty at an affordable price!

Газовая варочная панель Whirlpool GOR 6414/NB — купить в Интернет-магазин бытовой техники и электроники Салон Спектр в г. Владимире с доставкой. Характеристики, цена 23 353 руб. Whirlpool GOR 6414/NB, каталог, новинки, акции, кредит!

Варочная поверхность Whirlpool GOR 6414/NB - купить по цене от 10700 руб в интернет-магазинах Москвы, характеристики, фото, доставка

Whirlpool GOR 6414/NB купить в интернет-магазине: цены на варочная поверхность газовая GOR 6414/NB - отзывы и обзоры, фото и характеристики. Сравнить предложения в Украине: Киев, Харьков, Одесса, Днепр на Hotline.ua

Газова варильна поверхня Whirlpool GOR 6414/NB – фото, отзывы, характеристики в интернет-магазине ROZETKA от продавца: Life&land | Купить в Украине: Киеве, Харькове, Днепре, Одессе, Запорожье, Львове

Варочная поверхность WHIRLPOOL GOR 6414/NB - Купить в Киеве, Украине • Лучшая цена в интернет-магазине - tehnohata.ua

Варочная поверхность WHIRLPOOL GOR 6414/NB - Купить в Киеве, Украине • Лучшая цена в интернет-магазине - tehnohata.ua

Варочная поверхность Whirlpool GOR 6414/NB купить в Гомеле в рассрочку в интернет магазине с доставкой

Whirlpool GOR 6414/NB купить в интернет-магазине: цены на варочная поверхность газовая GOR 6414/NB - отзывы и обзоры, фото и характеристики. Сравнить предложения в Украине: Киев, Харьков, Одесса, Днепр на Hotline.ua
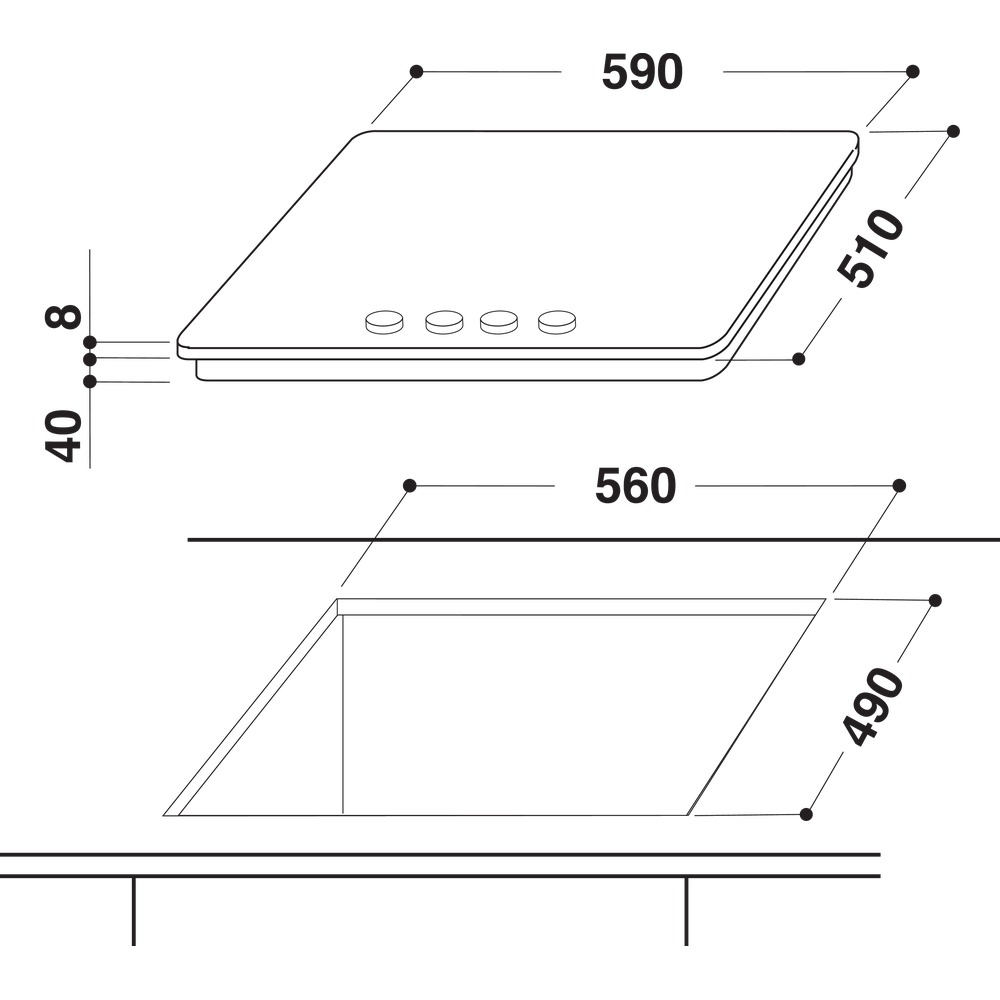
Whirlpool Egypt - Welcome to your home appliances provider - Whirlpool gas hob: 4 gas burners - GOR 6414/NB

Whirlpool GOR 6414/NB купить в интернет-магазине: цены на варочная поверхность газовая GOR 6414/NB - отзывы и обзоры, фото и характеристики. Сравнить предложения в Украине: Киев, Харьков, Одесса, Днепр на Hotline.ua

Накладка для плиты (духовки) Whirlpool 481010723544 купить в Киеве: цена и описание в гипермаркете Fix-Hub